Explore IL-23 inhibitors in psoriasis. Learn about clinical efficacy, dosing strategies, and how drugs like risankizumab and guselkumab help clear skin.
IL-23 Inhibitors in Psoriasis: Dosing Strategies and Clinical Efficacy
Imagine living with skin that stays clear long after your last treatment. This goal is becoming a reality for many people with psoriasis. New research shows how IL-23 inhibitors in psoriasis change lives. These drugs offer hope for long-term relief from red, itchy plaques. In this guide, you will learn about the latest dosing strategies and clinical efficacy of these treatments. We will explore how they work, how they are dosed, and what the future holds for psoriasis care.
How IL-23 Inhibitors in Psoriasis Work
Targeting the IL-23 Pathway
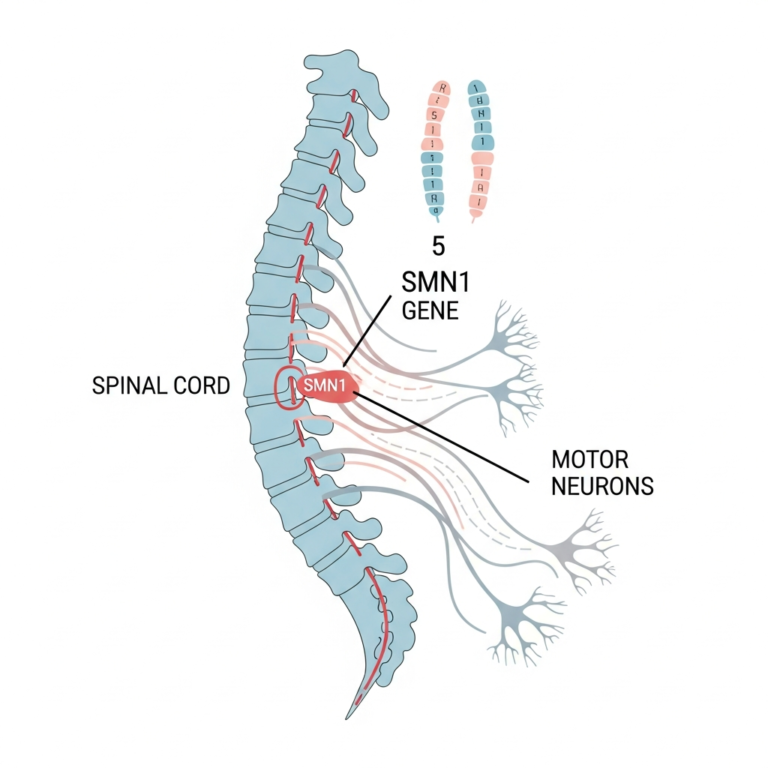
Psoriasis is an inflammatory skin disease. It causes red, scaly patches on the body. IL-23 inhibitors in psoriasis work by targeting a specific part of the immune system. Specifically, they block the IL-23p19 subunit. This subunit is a key driver of the inflammation that causes psoriasis symptoms. By blocking this pathway, these drugs can stop the inflammatory process at its source.
The Role of Resident Memory T Cells
A major challenge in psoriasis is recurrence. Plaques often return to the exact same spots on the skin. This happens because of resident memory T (TRM) cells. These cells stay in the skin even after it looks healed. IL-23 is a vital survival factor for these TRM cells. Therefore, clinical efficacy depends on reducing these cells to prevent flares.
Measuring Clinical Efficacy with PASI Scores
Doctors use the Psoriasis Area and Severity Index (PASI) to measure disease. The score ranges from 0 to 72. A score of 0 means no disease, while 72 is the most severe. When discussing clinical efficacy, researchers use percentage response rates. For example, PASI 100 means the skin is 100% clear. Achieving PASI 90 or 100 has a huge impact on a patient’s quality of life.
Advanced Dosing Strategies and Clinical Efficacy
The Concept of Dose-Spacing
Many patients want to reduce their treatment burden. Dose-spacing (D-S) is a strategy where doctors extend the time between injections. This is done for patients who have stable, clear skin. First, the patient must achieve a stable response, such as PASI 90 or 100, for at least six months. Next, the interval between doses is increased. This approach can save money and reduce the psychological burden of frequent injections.
Clinical Efficacy of Dose-Spacing Strategies
A recent study looked at risankizumab and guselkumab in a real-life setting. Patients in the study extended their dosing intervals by 50%. For guselkumab, this meant moving from every 8 weeks to every 12 weeks. For risankizumab, it meant moving from every 12 weeks to every 18 weeks. Finally, the results showed that 100% of the patients who were observed for 12 months maintained clear skin.
High-Dose Induction: The KNOCKOUT Trial
Another approach is to “hit hard and early”. The KNOCKOUT trial tested high induction doses of risankizumab. Patients received either 300 mg or 600 mg at weeks 0, 4, and 16. These doses are much higher than the standard 150 mg dose. The goal was to see if high doses could “knock out” TRM cells in the skin.
Long-Term Remission Results
The results of the high-dose trial were impressive. At week 28, 83% of patients reached PASI 100. Even more striking was the week 52 data. At that point, 43% of patients still had completely clear skin. This was nine months after their very last dose of medication. This study suggests that high-dose IL-23 inhibitors in psoriasis may induce long-term remission without constant dosing.
Comparative Clinical Efficacy of Leading Drugs
Risankizumab vs. Guselkumab
Both risankizumab and guselkumab are highly effective IL-23 inhibitors in psoriasis. However, there are some differences in how they work initially. In a pilot study, risankizumab provided a faster initial response. At week 16, 63% of risankizumab patients reached PASI 100. Only 28% of guselkumab patients reached the same goal in that timeframe. Furthermore, risankizumab showed better results at week 28 for PASI 90 achievement.
Long-Term Comparison and Stability
Despite the initial speed difference, both drugs are similar in the long run. After one year of dose-spacing, there were no significant differences in clinical efficacy. Both treatments kept the skin clear for the vast majority of patients. The drug survival rate for the dose-spaced regimen was about 89.4%. This means most patients did not need to return to standard dosing.
Who is a Candidate for These Dosing Strategies?
Not every patient is a fit for dose-spacing. Ideal candidates are “super responders” who reach clear skin quickly. Some factors may make dose reduction more difficult. For example, patients with obesity or psoriatic arthritis may have a lower response to treatment. These groups were under-represented in the dose-spacing studies. It is important to work with a doctor to find the best plan for your needs.
The Safety of IL-23 Inhibitors in Psoriasis
General Safety and Tolerability
Safety is a major concern for any long-term treatment. IL-23 inhibitors in psoriasis have a very favorable safety profile. They are often cited as having the lowest rates of adverse events among biologics. Common side effects are usually mild. These include upper respiratory infections, headaches, and fatigue. Injection site reactions like redness or pain are uncommon.
Adverse Events in High-Dose and Tapered Regimens
Research shows that even higher doses are well-tolerated. In the KNOCKOUT trial, no new safety signals were found with high-dose risankizumab. Similarly, dose-spacing did not lead to many adverse events. In one study, only two patients permanently stopped treatment due to side effects. One person experienced a migraine, and another reported joint pain. Overall, these drugs are considered safe for long-term use.
The Future of IL-23 Inhibitor Dosing Strategies
Moving Toward a Potential Cure
The goal of psoriasis research is changing. Instead of just managing symptoms, scientists are looking for a cure. By using the “hit hard and hit early” strategy, they hope to stop psoriasis from becoming a chronic disease. If TRM cells can be fully removed from the skin, long-term remission might become permanent.
Personalised Medicine and Monitoring
In the future, dosing may be even more personalised. Some doctors use blood tests to monitor drug levels. If a patient has high drug levels and clear skin, they may be a good candidate for a lower dose. This approach helps ensure that patients get exactly what they need without over-treating.
Conclusion: Summary of Clinical Efficacy
IL-23 inhibitors in psoriasis represent a massive leap forward in care. They target the root of inflammation and provide durable clearance. Whether through dose-spacing or high-dose induction, these dosing strategies offer new flexibility. Most importantly, they allow many patients to maintain PASI 100 results with fewer injections. As we learn more about TRM cells, the hope for long-term remission continues to grow.
FAQ: Common Questions About IL-23 Inhibitors
What are the most common IL-23 inhibitors?
The most common drugs in this class are risankizumab (Skyrizi) and guselkumab (Tremfya). These medications are specifically designed to block the IL-23 pathway to treat plaque psoriasis.
What is the standard dosing for these drugs?
Standard dosing for guselkumab is usually 100 mg every 8 weeks. For risankizumab, the standard dose is 150 mg every 12 weeks after an initial induction phase.
Can I safely reduce my dose?
Dose-spacing is a strategy used for patients who have had stable, clear skin for at least six months. However, you should never change your dose without consulting your dermatologist first.
Are high doses of risankizumab safe?
Yes, clinical trials like KNOCKOUT have shown that doses as high as 600 mg are well-tolerated. These studies found no new safety concerns when compared to standard doses.
How quickly do these drugs work?
Many patients see results by week 16. Risankizumab has been shown to work slightly faster for some, with 63% of patients reaching PASI 100 at that time.
Analogy for Understanding TRM Cells:
Think of resident memory T cells like dormant embers in a fireplace. Even after the fire (the psoriasis flare) is out, the embers remain hot. If they aren’t fully extinguished, they can easily start a new fire in the same spot. IL-23 inhibitors act like a bucket of water that cools those embers, preventing the fire from coming back.