Meta Title: Retinal Biomarkers for Cardiovascular Risk Stratification in the USA
Meta Description: Learn how retinal biomarkers and AI are transforming cardiovascular risk stratification in the USA with non-invasive eye imaging.
Introduction: The Eye as a Window to Heart Health
Heart disease remains the leading cause of death in the United States, yet many patients still slip through screening gaps. Traditional risk calculators, while helpful, can miss subtle vascular changes that occur years before symptoms manifest.
Oculomics is the emerging study of the eye as a mirror of systemic health. Because the retina is the only place in the human body where blood vessels can be visualized non-invasively, it serves as a “canary in the coal mine” for the heart.
The integration of deep learning and retinal biomarkers offers a faster, cheaper, and more accurate method for risk prediction. This article explores how AI enhancements and optometry clinics are revolutionizing cardiovascular screening in the USA.
Understanding Retinal Biomarkers for Cardiovascular Risk Stratification
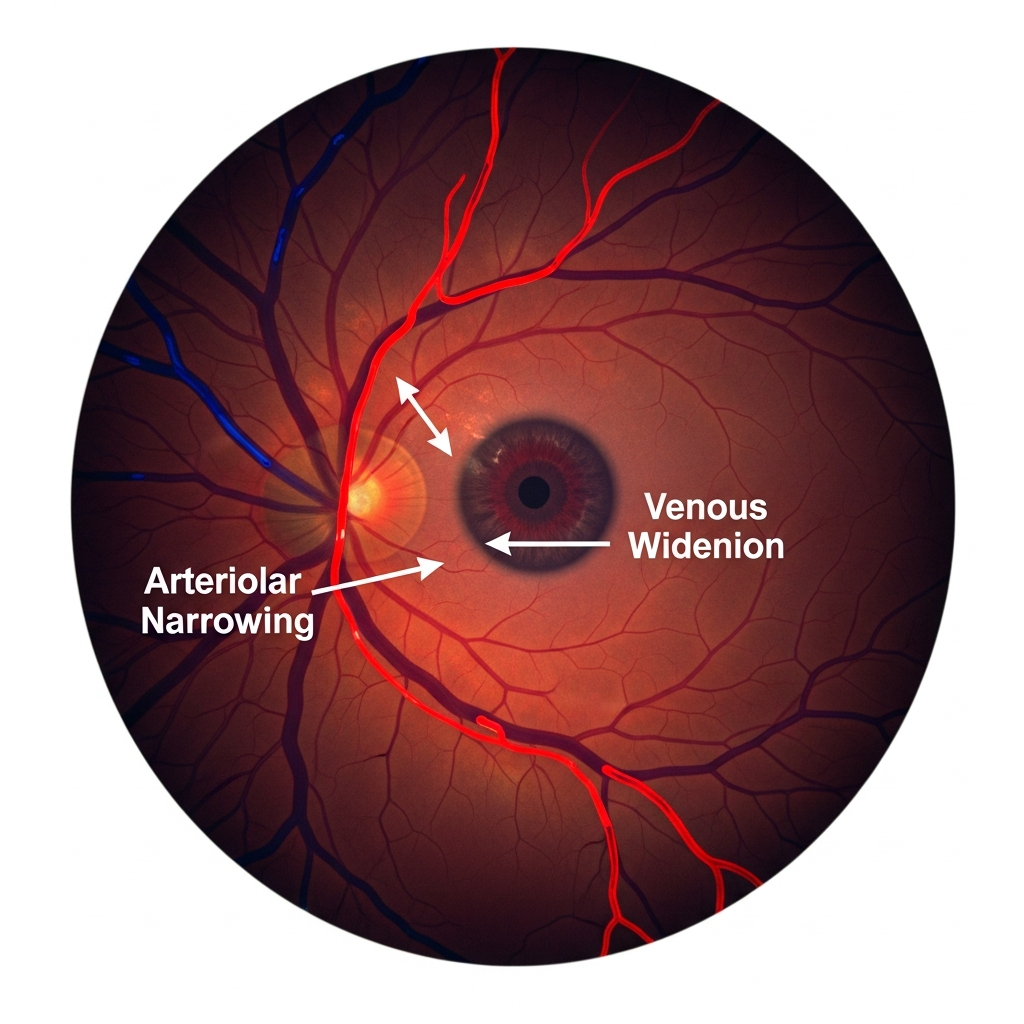
Retinal biomarkers are measurable traits in the eye’s blood vessels that reflect the state of the entire cardiovascular system. Clinicians use fundus photography to capture these specific traits:
Vessel Calibre and Width: Narrow arteries and widened veins are classic indicators of hypertension and vascular stress.
Vessel Tortuosity: Increased “twistiness” reflects endothelial stress, while unusually straight vessels can signal long-term hypertension.
Fractal Dimension (FD): A lower FD, known as “rarefaction,” suggests microvascular damage and a loss of vascular complexity.
Arterio-Venous Ratio (AVR): This is a cornerstone biomarker. A low AVR is a strong predictor of potential stroke and coronary heart disease.
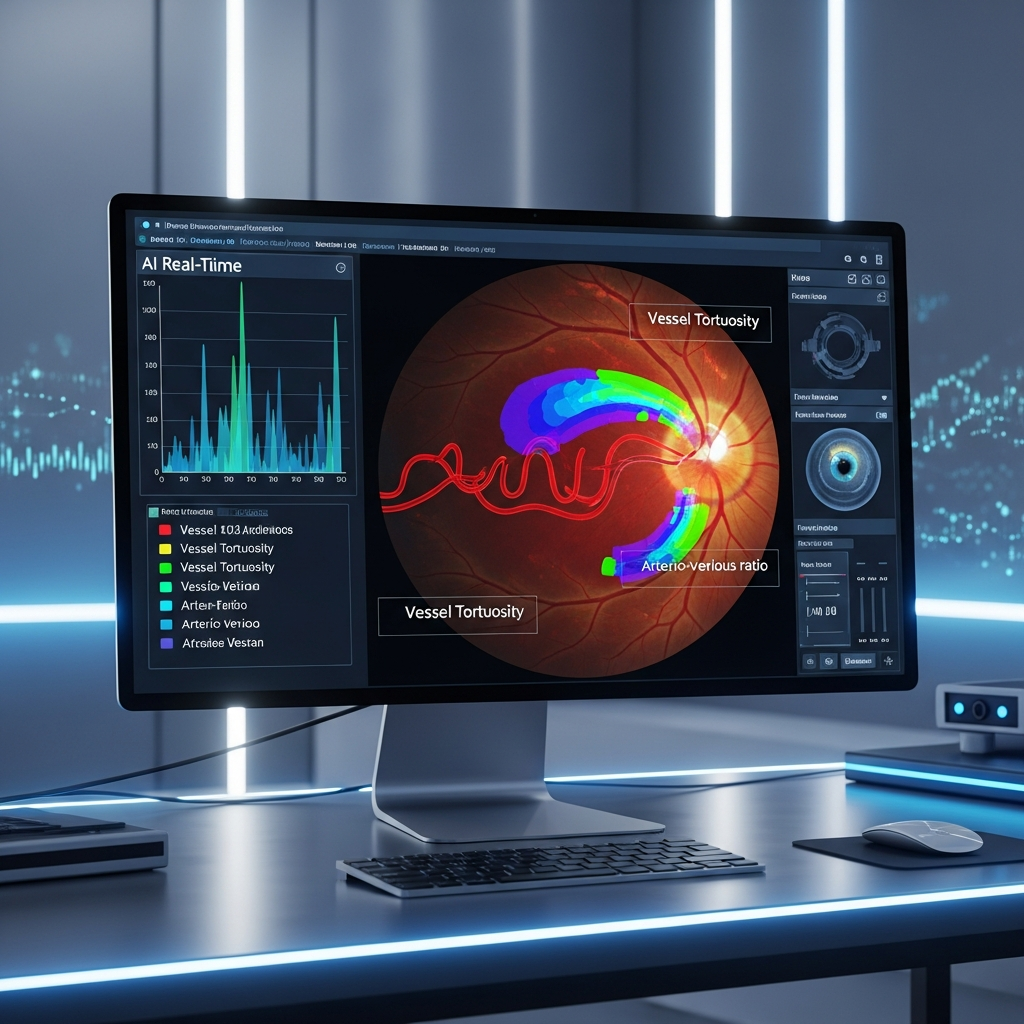
How AI Enhances Cardiovascular Risk Stratification
Artificial intelligence is transforming oculomics from a manual observation into a precise science. Deep learning models, such as Reti-CVD, analyze retinal images with accuracy levels comparable to expensive CT-based approaches.
High Performance: AI shows high sensitivity for identifying intermediate-to-high risk groups.
Inferring Systemic Factors: Beyond just looking at vessels, AI can infer a patient’s biological age, gender, smoking status, and systolic blood pressure just from retinal features.
Early Intervention: AI detects risk in asymptomatic patients, allowing for lifestyle changes before a cardiac event occurs.
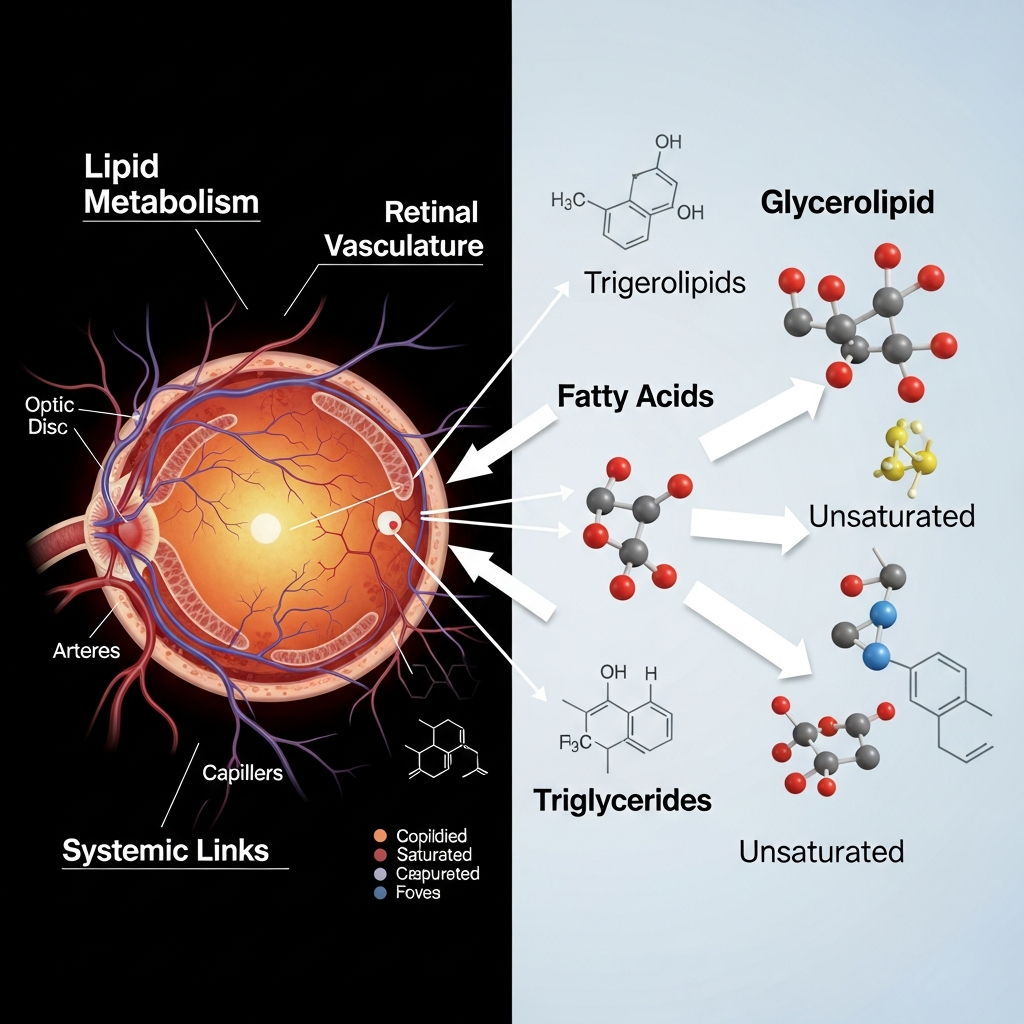
Beyond Imaging: Linking Retinal Traits to Systemic Lipid Profiles
The next frontier of oculomics connects retinal traits with lipidomics—linking eye health directly to metabolic function.
Glycerolipids (DAG and TAG): Elevated levels are associated with arterial narrowing and “rarefaction” (thinning) of the vessel network.
Fatty Acids (FA): High FA levels correlate with reduced vessel tortuosity—resulting in straighter vessels that indicate higher cardiovascular risk.
By combining lipidomics with retinal biomarkers, healthcare providers can detect molecular dysfunction long before clinical disease appears.
Integrating Retinal Risk Stratification into Primary Care
Optometry clinics are the ideal frontline for cardiovascular screening. Since many Americans visit their eye doctor more regularly than a specialist, these clinics can bridge the “attendance gap.”
Co-management: Establishing clear referral pathways between optometrists and cardiologists ensures patients get help early.
Red Flags: Conditions like Retinal Vein Occlusion (RVO) or Diabetic Retinopathy (DR) should be treated as immediate signals for a comprehensive cardiovascular workup.
Conclusion: The Future of Preventative Cardiovascular Care
Retinal imaging is validated, scalable, and cost-effective. By utilizing the eye as a diagnostic tool, USA healthcare providers can detect risks earlier, reduce costs, and improve long-term patient outcomes.
Analogy for Understanding
Retinal vessels are like a car’s tailpipe. By inspecting the exhaust—the eye—you can tell how well the engine—the heart—is running, without having to open the hood.
Frequently Asked Questions (FAQ)
Can an eye test really predict a heart attack?
Yes. Microvascular changes and AI analysis of the retina can predict 5-year risks for major cardiac events.
What is “Life’s Simple 7” (LS7)?
These are seven key metrics—diet, activity, weight, smoking, blood pressure, cholesterol, and glucose—that reduce both heart disease and sight-threatening eye conditions.
How accurate is AI compared to traditional blood tests?
AI-based retinal analysis (like Reti-CVD) shows sensitivity and specificity levels comparable to the gold-standard QRISK3 blood-based assessments.