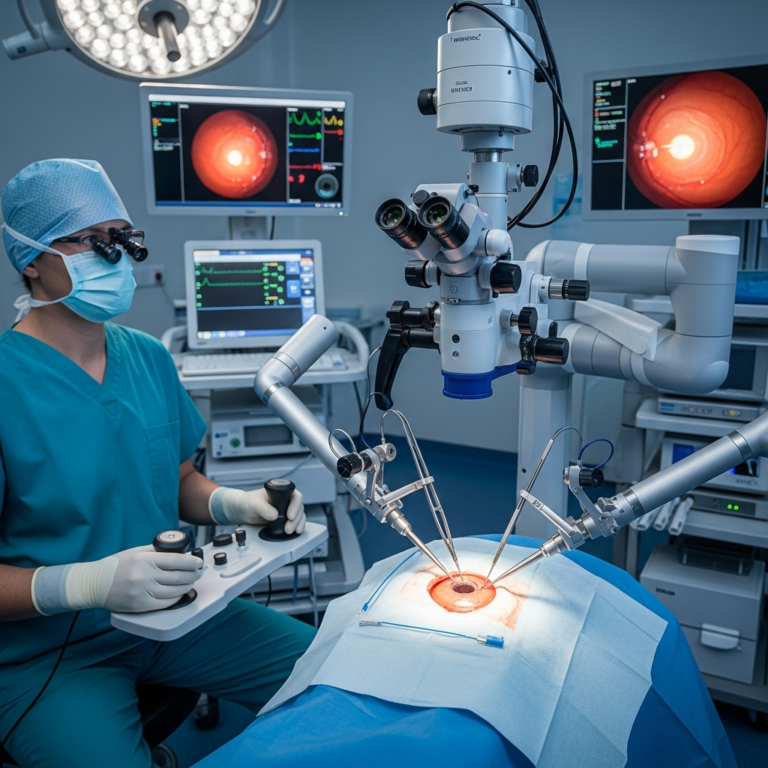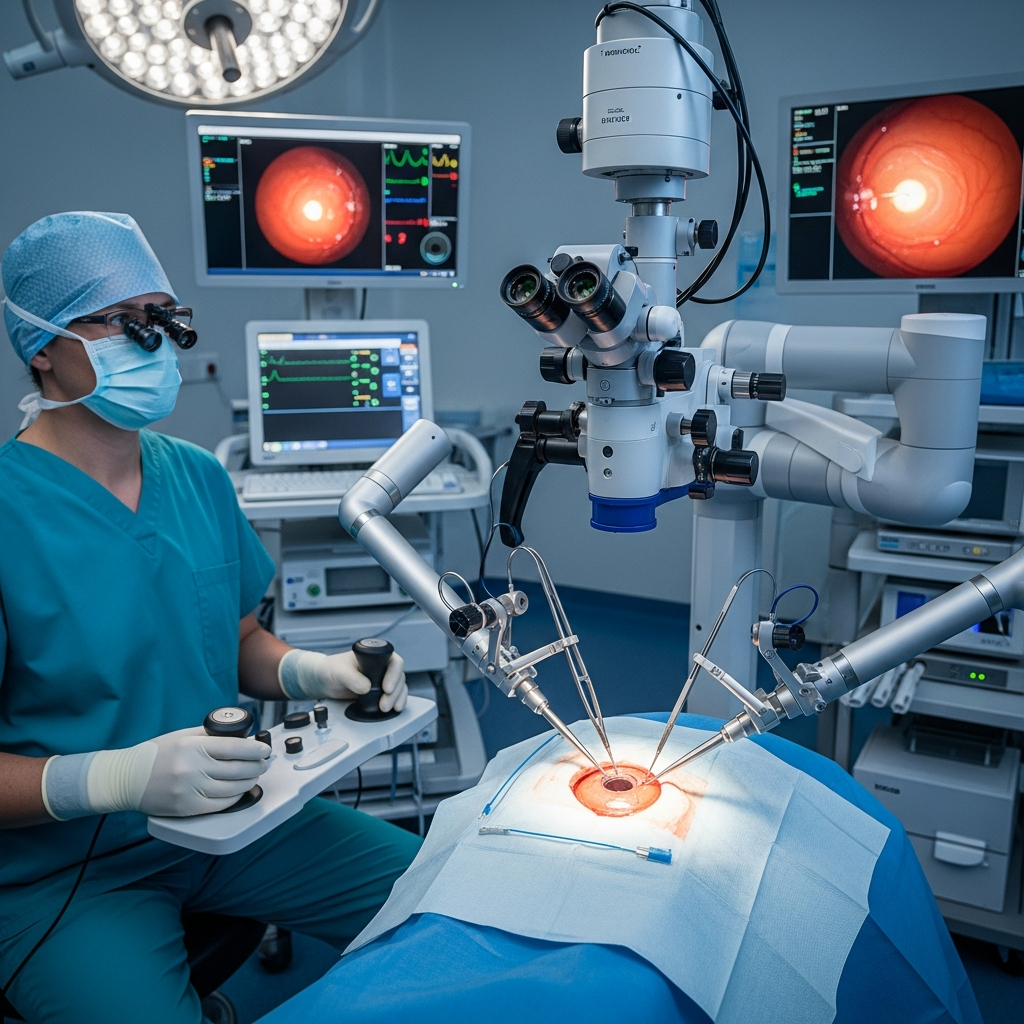
Robotic systems enhance surgical precision in delicate ophthalmic procedures.
Advancements in Robotic Assistance for Ophthalmic Microsurgery
Human hands are amazing, but they have physical limits. In the world of eye surgery, those limits are a major challenge. Surgeons often work on structures thinner than a human hair. Even the best surgeons have tiny, involuntary hand tremors. These tremors average about 180 microns in size. However, the light-sensitive layer of the retina is only about 200 microns thick.
In this article, you will learn about the latest advancements in robotic assistance for ophthalmic microsurgery. We will cover the new robotic systems being used today. You will also discover how Artificial Intelligence (AI) is making these procedures safer. Finally, we will look at how robots help surgeons perform tasks that were once thought impossible.
Why Do We Need Advancements in Robotic Assistance for Ophthalmic Microsurgery?
The eye is a very delicate organ. Modern eye surgery requires incredible precision. When a surgeon operates on the retina, there is almost no sense of touch. They must rely entirely on what they see through a microscope.
The Problem with Human Limitations
First, humans naturally tremble. These “physiologic tremors” are usually invisible to the naked eye. But under a surgical microscope, they become a problem. Fatigue also plays a role. Longer surgeries can make a surgeon’s hand less steady.
How Robots Fill the Gap
Robots do not get tired. They can also filter out hand tremors. These systems take a surgeon’s movement in millimetres and translate it into micrometres. This is called motion scaling. It allows for much finer control than a human hand could ever achieve alone.
Leading Systems in Robotic Ophthalmic Surgery
Several companies are leading the way in this field. Each system offers unique tools to help the surgeon.
The PRECEYES Surgical System
The PRECEYES Surgical System is a top robotic assistant. It provides precision better than 20 microns. This system acts like a “mechanical hand” with seven motors. It can hold a needle perfectly still for long periods. If the surgeon lets go of the joystick, the robot “freezes” the instrument in place for safety.
The ForSight Robotics ORYOM Platform
The ORYOM platform is another major breakthrough. It is the world’s first hybrid robotic platform for eye surgery. It features a miniature robotic hand with 14 degrees of freedom. This allows it to reach almost any location within the human eye. It is designed for high-volume procedures like cataracts and glaucoma.
The Da Vinci Xi System
While originally made for larger surgeries, the Da Vinci Xi is now being tested for the eye. Researchers used it to perform cornea transplants on human tissue. The robot’s improved optics and microsurgical tools allowed it to complete the surgery in about 43 minutes. This is very close to the time it takes a human to do it manually.
Breakthrough: Retinal Vein Cannulation (RVC)
One of the most exciting advancements in robotic assistance for ophthalmic microsurgery is in treating Retinal Vein Occlusion (RVO). RVO happens when a vein in the retina becomes blocked. This can lead to blindness.
The Challenge of RVC
To treat this, surgeons try to insert a tiny needle into the blocked vein to deliver medicine. This is called retinal vein cannulation (RVC). These veins are as thin as a human hair. Manually holding a needle inside such a small vein for 10 minutes is nearly impossible for a human.
Robotic Success in RVC
Robots make this procedure feasible. In a world-first trial, surgeons used a robot to safely inject medicine into a 100-micron-thick vein for 10 minutes. Robotic systems ensure the needle stays perfectly still. This prevents the needle from puncturing through the other side of the fragile vein.
How AI and Deep Learning are Changing Eye Care
AI is now being used to guide robotic surgical tools. This is a major step toward autonomous surgery.
Real-Time Tracking with iOCT
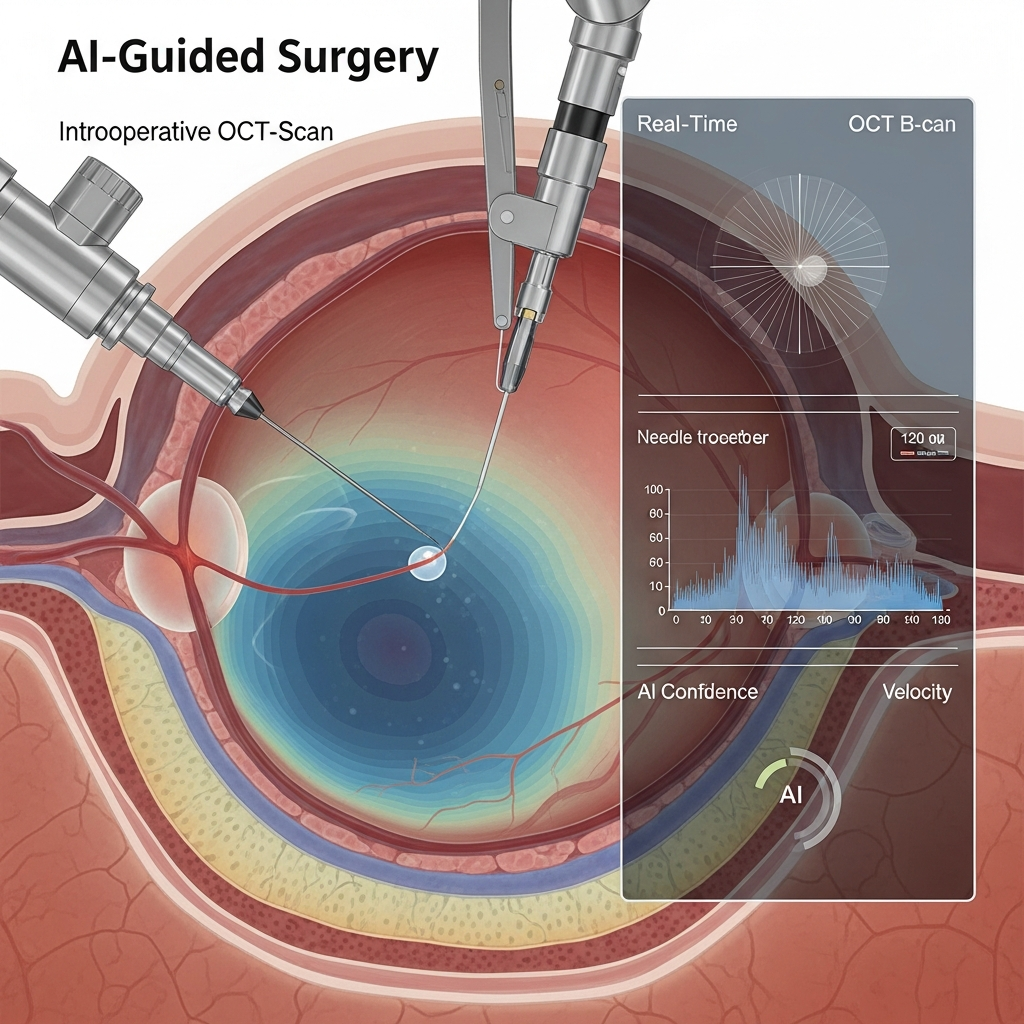
Researchers at Johns Hopkins University developed a system guided by deep learning. It uses a tool called intraoperative Optical Coherence Tomography (iOCT). Think of iOCT as a “depth sensor”. It provides cross-sectional views of the eye tissue in real-time.
Autonomous Precision
The AI tracks the needle tip and the layers of the retina automatically. In tests on pig eyes, this autonomous system achieved a 90% success rate for needle insertion. The average accuracy was within 26 microns. This level of precision is much higher than what most human surgeons can achieve manually.
Safety and the “No-Fly Zone”

Safety is the biggest priority in advancements in robotic assistance for ophthalmic microsurgery. Robots can be programmed with safety constraints.
- Remote Centre of Motion (RCM): This ensures the surgical tool only moves around the entry point in the eye. This prevents the robot from putting pressure on the eye wall, which could cause damage.
- No-Fly Zones: Robots can be programmed to “ignore” a command if it would cause the tool to touch a dangerous area. For example, if a surgeon accidentally moves toward the delicate endothelium, the robot will simply stop.
- Speed of Reaction: If a patient moves, a human surgeon might react in 250 milliseconds. A robot can react and pull the tool out in just 20 milliseconds.
Lifestyle Factors: Can We Improve Human Performance?
While robots are the future, there are ways to improve human steadiness today. A systematic review identified several factors that affect a surgeon’s tremor.
Diet and Caffeine
Caffeine has been shown to increase hand tremors. Studies found that coffee can have a negative effect on a surgeon’s performance in simulators. It is recommended to avoid caffeine right before surgery.
Medication and Exercise
Some surgeons use beta-blockers like Propranolol to reduce tremors. These can decrease tremor magnitude by about 22%. Exercise is also a factor. High-intensity workouts can increase tremors for up to 4 hours after the session.
Yoga and Breathing
New research suggests that yoga and deep breathing (Pranayama) can help. These exercises have been shown to decrease micro-tremors in young surgeons. They also help reduce stress, which is a common cause of shakiness.
Professional Opinion: The Future of the Operating Theatre
As an expert partner in this discussion, it is clear that we are entering a “hybrid” era of eye care. Robots are not replacing surgeons yet. Instead, they are becoming high-tech extensions of the surgeon’s own hands.
The most significant impact will likely be in “impossible” surgeries. Procedures like subretinal drug delivery and complex vein cannulation require a level of stillness that biology simply does not provide. While the high cost of these robots is currently a barrier, the efficiency they bring could eventually lower costs by automating simple parts of high-volume surgeries like cataracts.
The integration of AI is the most promising advancement. It removes the “guesswork” from depth perception. In my view, the “no-fly zone” safety feature alone makes a strong case for the widespread adoption of these systems in training hospitals.
Conclusion
The advancements in robotic assistance for ophthalmic microsurgery are moving fast. We have gone from simple tools to autonomous systems guided by AI. These robots filter out tremors, scale movements, and provide real-time depth data. They allow us to treat diseases like Retinal Vein Occlusion with world-first precision.
While we are not yet at the point of fully robotic clinics, the technology is no longer a fantasy. It is a real tool saving people’s sight today.
FAQ
Q: Will robots eventually replace eye surgeons?
A: Most experts say no. Robots are designed to enhance a surgeon’s skill, not replace their clinical judgment. We are “nowhere near being obsolete”.
Q: Can a robot perform eye surgery completely on its own?
A: There are prototypes for autonomous surgery, but they still require a surgeon to supervise from a separate room. Currently, most systems are surgeon-controlled.
Q: Is robotic eye surgery currently available to the public?
A: In a limited scope, yes. Systems like the Preceyes and AcuSurgical are in human use outside of the United States. Other systems are still in the clinical trial phase.
Q: Why are robots slower than human surgeons?
A: Modern robotic systems are still in the early stages. They are currently slower because of the high level of caution and setup time required. They are expected to get faster as AI learns from more procedures.
References
- : “A new robotic system could perform delicate eye surgery,” Medical Xpress (2026).
- : “Da Vinci Xi Robot–Assisted Penetrating Keratoplasty,” PMC (2017).
- : “Deep Learning Guided Autonomous Retinal Surgery,” arXiv (2020).
- : “ForSight Robotics raises $125M to advance robotic platform,” Eyes On Eyecare (2026).
- : “In-Human Robot-Assisted Retinal Vein Cannulation, A World First,” Ann Biomed Eng (2018).
- : “Ophthalmology: Say Hello to Robotic Surgery,” AAO (2024).
- : “Overcoming the impact of physiologic tremors in ophthalmology,” PMC (2022).
- : “Preceyes Surgical System Product Details,” Preceyes B.V. (2022).
- : “Robot helps in delicate eye operation,” ICT&health (2016).
- : “Robotic eye surgery – an overview,” EuroEyes (2019).